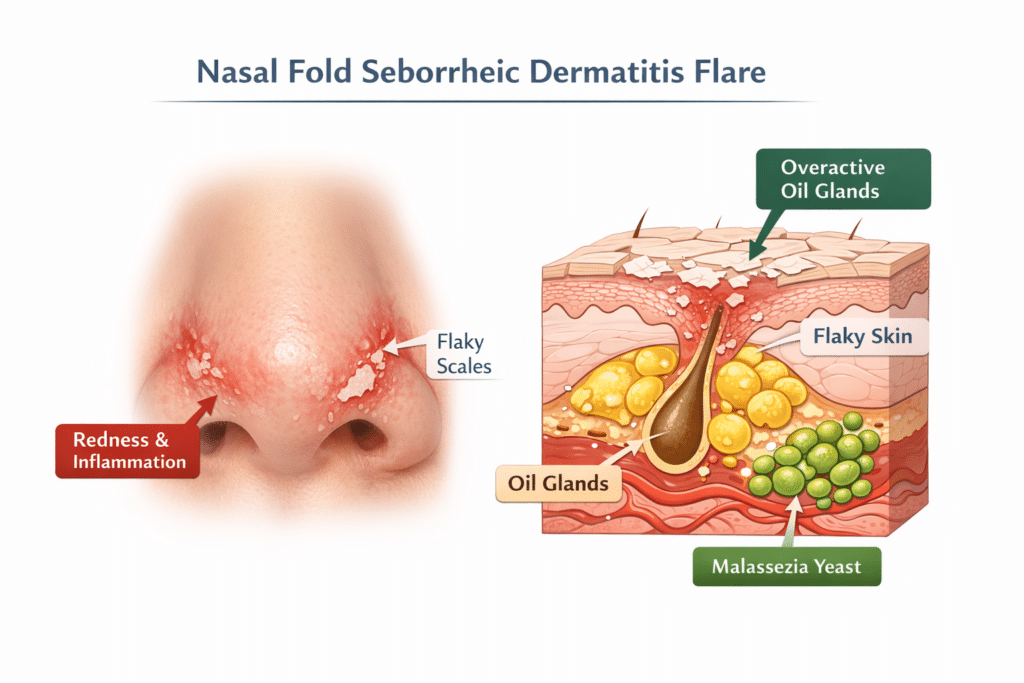
Seborrheic dermatitis around the nose is one of the most common facial flare areas. The skin beside the nostrils and inside the nasal folds can become red, flaky, greasy, and irritated. Because this area naturally produces more oil than other parts of the face, it creates an environment where inflammation can easily develop.
For many people, this flare pattern is confusing. It may look like dry skin. It may feel like an allergic reaction. Some mistake it for acne or eczema. In reality, it follows a predictable pattern once you understand what’s happening under the surface.
Seborrheic dermatitis is a broader condition that can affect multiple areas of the body for a full understanding of causes, symptoms and treatment see our seborrheic dermatitis guide.
Why the nose is a hotspot for flare-ups
The folds beside the nose contain a high concentration of oil glands. These glands produce sebum, which helps protect the skin. However, sebum also feeds a naturally occurring yeast called Malassezia.
This yeast is present on everyone’s skin. It is not an infection. It is not contagious. The problem is not the yeast itself it is the immune response.
In people prone to seborrheic dermatitis:
- the immune system reacts too strongly
- inflammation is triggered
- skin turnover accelerates
- flakes and redness appear
The nasal folds also trap warmth and moisture. Add friction from tissues, wiping the nose, winter illness, or allergies, and the skin barrier becomes even more vulnerable.
This combination explains why the nose is often the first facial area to flare.
This confusion is common. For example, contact dermatitis rash is triggered by external irritation, while conditions affecting oil-rich areas follow a different pattern.
Perioral dermatitis is another condition that can affect this area, particularly around the mouth and nose, and can sometimes be mistaken for seborrheic dermatitis.
Seborrheic dermatitis can affect both the face and scalp, often as part of the same condition.
Common symptoms around the nose
Symptoms tend to cycle. They flare, settle, then return. Many people describe a pattern that worsens in winter, during stress, or when sick.
Typical signs include:
- redness in the folds beside the nostrils
- yellow or white flaky patches
- greasy or shiny skin texture
- itching that comes and goes
- burning or stinging sensation
- skin that reacts to skincare or makeup
- scaling that reappears after washing
While symptoms often begin around the nose, they frequently extend to other areas. Seborrheic dermatitis on the scalp is one of the most common related patterns.
Unlike simple dryness, seborrheic dermatitis rarely disappears with moisturiser alone. The inflammation component must also be addressed.
Symptoms often extend beyond the nasal folds. Seborrheic dermatitis on the face can affect a wider area, including the eyebrows and forehead.
While symptoms often begin around the nose, they frequently extend to other areas. Seborrheic dermatitis on the scalp is one of the most common related patterns; for in-depth advice on managing these, you can explore our guide on effective scalp seborrheic dermatitis treatments.
What makes flare-ups worse
Understanding triggers is one of the strongest prevention tools.
Common aggravators include:
- cold weather and indoor heating
- illness or immune stress
- emotional stress
- harsh cleansers
- fragranced skincare
- alcohol-based toners
- scrubbing or exfoliating
- heavy occlusive makeup
- over-washing the face
- wiping the nose frequently
Many people accidentally worsen symptoms by trying to scrub flakes away. This damages the barrier and fuels the cycle.
Gentle care is more effective than aggressive treatment.
For daily support, many people use a gentle routine like our scalp care range for seborrheic dermatitis
A simple routine that actually helps
| Time | Step | What to Do | Why It Matters |
|---|---|---|---|
| Morning | Cleanse | Use a gentle, fragrance-free cleanser | Removes oil without stripping skin |
| Dry | Pat dry - do not rub | Prevents irritation in inflamed areas | |
| Moisturise | Apply a soothing barrier cream | Calms redness and supports repair | |
| Protect | Use mineral sunscreen | Shields sensitive skin from irritation | |
| Evening | Cleanse | Wash gently again | Clears buildup from the day |
| Treat (if flaring) | Short-contact antifungal wash | Helps control yeast overgrowth | |
| Moisturise | Apply immediately after cleansing | Locks in hydration | |
| Simplify | Keep routine minimal | Overuse worsens irritation |
Many people also benefit from using gentle, barrier-supporting creams designed for sensitive skin to help calm irritation and maintain hydration between flare-ups.
How antifungal washes fit in
Short-contact antifungal treatment is often helpful during active flares.
These include products with:
- ketoconazole
- zinc pyrithione
- selenium sulphide
Use 2–3 times per week:
- apply to damp skin
- leave for 30–60 seconds
- rinse thoroughly
- moisturise after
This is not a daily long-term step. It is a flare control tool.
Overuse can dry the skin.
Balance matters.
Long-term maintenance strategy
Seborrheic dermatitis is chronic. It tends to return. The goal is control, not permanent cure.
Maintenance focuses on:
- gentle daily cleansing
- consistent moisturising
- stress management
- trigger awareness
- early flare treatment
- barrier protection
Think of it like asthma for the skin.
You manage patterns. You reduce severity. You shorten flares.
Many people achieve long periods of clear skin once they learn their triggers.
Seasonal care differences
Winter often worsens symptoms because:
- cold air dries skin
- heating reduces humidity
- illness increases inflammation
During winter:
- moisturise more frequently
- use humidifiers if possible
- avoid hot water washing
- protect skin outdoors
Summer can also trigger flares through:
- sweating
- sunscreen reactions
- increased oil production
Lightweight, non-comedogenic moisturisers work best in warm weather.
Adjusting routines by season prevents escalation.
Mistakes that prolong flare-ups
| Avoid | Why |
|---|---|
| Scrubs | Causes micro-damage to fragile skin |
| Acids | Increases burning and peeling |
| Retinoids | Too strong for inflamed skin |
| Essential oils | Common irritation trigger |
| Fragranced creams | Weakens skin barrier |
These are extremely common:
- scrubbing flakes away
- switching products constantly
- using acne treatments on inflamed skin
- over-cleansing
- ignoring early signs
- applying steroid creams too often
- layering too many actives
- trying to “dry out” the skin
Seborrheic dermatitis is not a hygiene problem.
It is an inflammatory barrier disorder.
Calming is more effective than attacking.
Recovery timeline and expectations
Many people expect overnight results. That leads to frustration.
Realistic improvement looks like:
- 1 week: reduced itching
- 2 weeks: less redness
- 3–4 weeks: visible calming
- 6 weeks: stabilisation
Consistency matters more than intensity.
Relapses are normal.
Quick response prevents escalation.
You can view our atopic cream for damaged or sensitive skin here.
When to seek medical advice
Professional care is important if:
- symptoms spread beyond the nose
- skin becomes painful
- infection appears
- scaling becomes thick
- over-the-counter care fails
- flares are frequent or severe
Prescription antifungals or anti-inflammatory creams may be needed in stubborn cases.
There is no failure in seeing a dermatologist.
It is part of proper management.
Psychological reassurance
Facial skin conditions affect confidence more than people admit.
Redness around the nose is highly visible. It can feel embarrassing. Many people withdraw socially during flares.
It’s important to understand:
- this condition is common
- it is not contagious
- it is manageable
- it does not reflect hygiene
- it improves with knowledge
Control comes from understanding patterns, not fighting your skin.
Many people feel like they are doing something wrong when flare-ups happen. In reality, seborrheic dermatitis behaves in cycles, and learning how to manage it is far more effective than trying to eliminate it completely.
Prevention mindset
Long-term success comes from:
- recognising early signs
- treating gently and early
- maintaining routine
- avoiding panic changes
- supporting the barrier
- accepting the cycle
Seborrheic dermatitis behaves predictably once understood.
The goal is stability, not perfection.
Frequently Asked Questions (Meta Version)
Is seborrheic dermatitis around the nose permanent?
Seborrheic dermatitis is a chronic condition, but it can be effectively managed. With consistent care, many people experience long periods without symptoms.
Why does seborrheic dermatitis keep returning around the nose?
The area around the nose has a high concentration of oil glands, creating an environment where flare-ups can easily recur.
Can moisturiser alone treat seborrheic dermatitis?
Moisturiser supports the skin barrier, but flare-ups often require antifungal or anti-inflammatory treatment to fully calm symptoms.
Does makeup make seborrheic dermatitis worse?
Yes, heavy or fragranced makeup can trigger irritation. Using lightweight, non-comedogenic products is generally safer.
Can stress trigger seborrheic dermatitis flare-ups?
Yes, stress is a common trigger and is strongly linked to increased flare-ups and symptom severity.
Should you exfoliate seborrheic dermatitis flakes?
No, exfoliating or scrubbing can worsen inflammation and delay healing. Gentle care is recommended instead.
Is seborrheic dermatitis the same as eczema?
No, although they share similarities. Seborrheic dermatitis is linked to yeast-related inflammation, while eczema involves a broader range of triggers.

